What Is the Credentialing Process in Delaware?
Table of Contents
ToggleThe credentialing process in Delaware is a formal verification system that confirms healthcare providers are qualified, licensed, and eligible to deliver medical services. It ensures patient safety and compliance with state and federal regulations.
If you plan to practice medicine, join an insurance network, or work in a hospital in Delaware, credentialing is not optional—it’s required.
This process matters because it directly impacts:
- Patient trust and safety
- Legal compliance
- Insurance reimbursements
- Professional credibility
What does credentialing mean in Delaware healthcare?
Credentialing is the process of verifying a healthcare provider’s qualifications, including education, training, licenses, and work history.
In Delaware, credentialing ensures that providers meet standards set by regulatory bodies and insurance payers.
Key elements include:
- License verification
- Board certification validation
- Education confirmation
- Employment history review
- Malpractice history check
Credentialing is required before:
- Joining hospitals
- Billing insurance companies
- Participating in Medicaid/Medicare
Who needs to complete the credentialing process in Delaware?
Any licensed healthcare professional must complete credentialing before practicing or billing insurers.
Common professionals include:
- Physicians (MD, DO)
- Nurse practitioners (NPs)
- Physician assistants (PAs)
- Psychologists and therapists
- Dentists
- Chiropractors
Even telehealth providers serving Delaware patients may need to be credentialed depending on payer requirements.
Which organizations regulate credentialing in Delaware?
Credentialing in Delaware involves multiple regulatory and oversight bodies.
Primary organizations include:
- Delaware Division of Professional Regulation (DPR)
- National Practitioner Data Bank (NPDB)
- Centers for Medicare & Medicaid Services (CMS)
- Private insurance companies
Each entity plays a role:
- DPR handles licensing
- NPDB tracks malpractice and disciplinary actions
- CMS manages Medicare enrollment
- Insurers conduct their own credentialing reviews
What are the main steps in the credentialing process in Delaware?
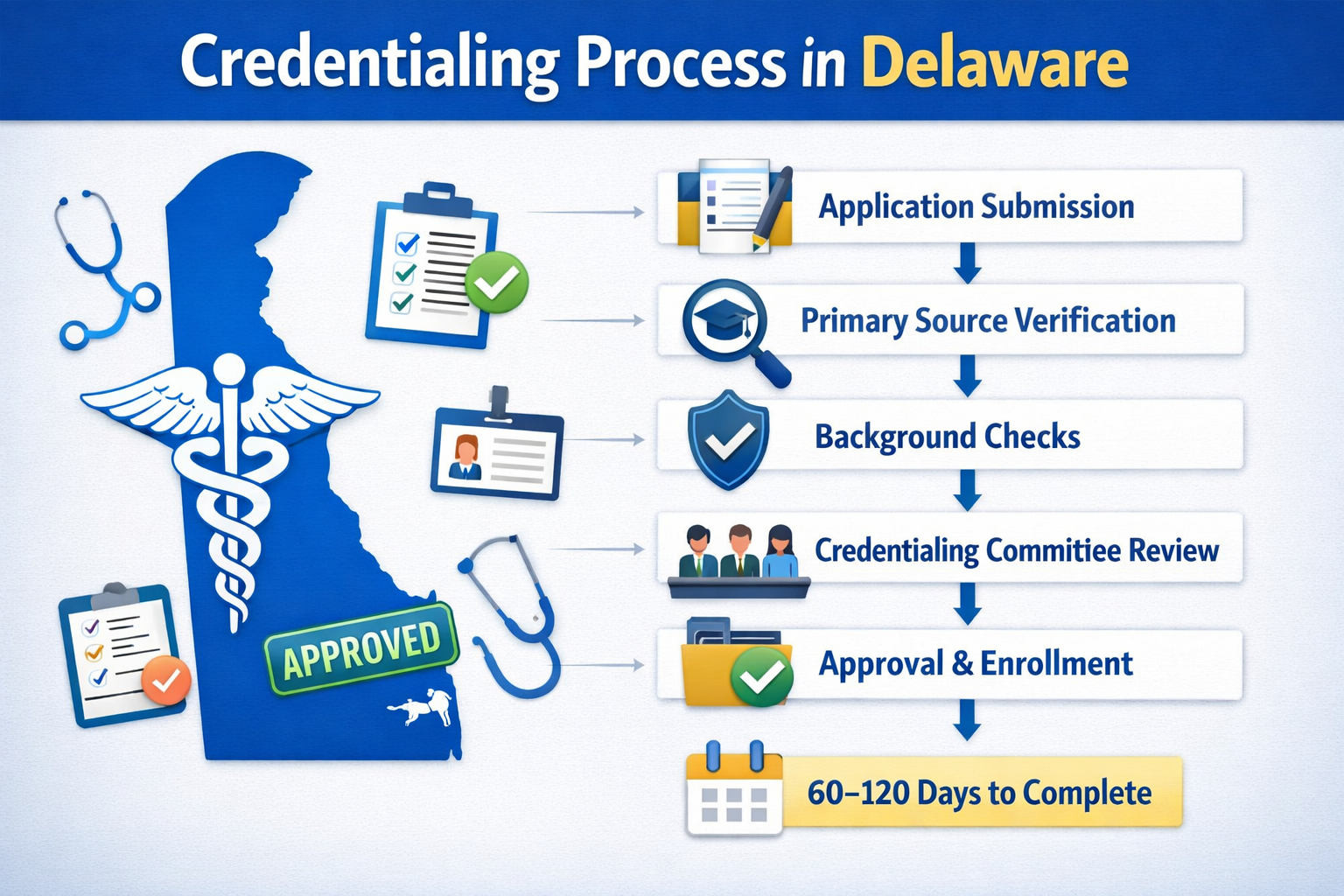
The credentialing process follows a structured workflow to ensure accuracy and compliance.
Core steps include:
- Application submission
- Document collection
- Primary source verification
- Background checks
- Committee review
- Approval and enrollment
What is primary source verification in credentialing?
Primary source verification (PSV) is the process of confirming credentials directly with the original issuing organizations.
Examples:
- Verifying medical school with the university
- Checking licenses with the state board
- Confirming board certification with certifying bodies
PSV is critical because it prevents fraud and ensures authenticity.
What happens during credentialing committee review?
A credentialing committee reviews the verified information and decides whether to approve the provider.
They evaluate:
- Professional competence
- Work history gaps
- Malpractice claims
- Ethical conduct
Approval allows the provider to:
- Join networks
- Start billing insurance
- Practice within facilities
What documents are required for credentialing in Delaware?
Credentialing requires a comprehensive set of documents to verify qualifications.
Typical documents include:
- State medical license
- DEA registration (if applicable)
- Board certification
- Resume/CV
- Malpractice insurance certificate
- Work history (last 5–10 years)
- Government-issued ID
Incomplete documentation is one of the biggest causes of delays.
How long does credentialing take in Delaware?
Credentialing in Delaware typically takes 60 to 120 days, depending on the organization and completeness of the application.
Factors affecting timeline:
- Insurance company processing speed
- Accuracy of submitted documents
- Responsiveness to verification requests
- Background check results
Medicare enrollment can take longer due to federal processing requirements.
How does insurance credentialing work in Delaware?
Insurance credentialing allows providers to bill insurance companies and receive reimbursement.
Process includes:
- Submitting applications to insurers
- Completing the CAQH profile
- Undergoing payer-specific verification
- Receiving network participation approval
Without insurance credentialing, providers may only accept self-pay patients.
What is CAQH, and why is it required?
CAQH (Council for Affordable Quality Healthcare) is a centralized database used by insurers to collect provider information.
Why it matters:
- Reduces duplicate paperwork
- Speeds up credentialing
- Standardizes provider data
Providers must:
- Create a CAQH profile
- Upload documents
- Keep information updated
What is the difference between credentialing and licensing in Delaware?
Credentialing and licensing are related but different processes.
| Aspect | Licensing | Credentialing |
|---|---|---|
| Purpose | Legal permission to practice | Verification of qualifications |
| Issued by | State board | Employers/insurers |
| Required for | Practicing legally | Billing and employment |
| Frequency | One-time with renewals | Ongoing (recredentialing) |
Licensing is mandatory to practice, while credentialing is required to work within systems and receive payments.
What are the common challenges in the credentialing process?
Credentialing delays are common but avoidable.
Top challenges include:
- Missing documents
- Incomplete applications
- Delayed responses from institutions
- Errors in CAQH profiles
- Work history gaps
Example:
A missing malpractice certificate can delay approval by weeks.
How much does credentialing cost in Delaware?
Credentialing costs vary depending on how it’s handled.
Typical cost ranges:
- Self-managed: minimal (time investment)
- Credentialing service: $100–$500 per application
- CAQH: free for providers
Additional costs may include:
- Licensing fees
- Background checks
- Insurance enrollment fees
What is recredentialing, and how often is it required?
Recredentialing is the periodic review of a provider’s qualifications.
Typically required every 2–3 years.
It ensures:
- Continued compliance
- Updated credentials
- Ongoing professional competence
Failure to recredential can result in removal from insurance networks.
What are the best practices to speed up credentialing in Delaware?
The fastest way to complete credentialing is to stay organized and proactive.
Best practices:
- Keep documents updated
- Complete the CAQH thoroughly
- Respond quickly to requests
- Track application status
- Use credentialing software or services
Pro tip:
Start credentialing 3–6 months before your intended start date.
Start Your Credentialing in Delaware with Vital Health Services
Key Takeaways
- Credentialing verifies a healthcare provider’s qualifications.
- It is required for insurance billing and hospital privileges.
- The process typically takes 60–120 days.
- CAQH plays a central role in insurance credentialing.
- Staying organized can significantly reduce delays.
FAQs
What is credentialing in Delaware?
Credentialing is the process of verifying a healthcare provider’s qualifications to ensure they meet professional standards.
How long does credentialing take?
It usually takes 60 to 120 days, depending on the organization and completeness of documents.
Is CAQH required for credentialing?
Yes, most insurance companies require a completed CAQH profile.
Can I work while waiting for credentialing?
You may work, but you typically cannot bill insurance until credentialing is complete.
How often is recredentialing required?
Recredentialing is usually required every 2 to 3 years.
What causes delays in credentialing?
Common causes include missing documents, incomplete applications, and slow verification responses.
Do all healthcare providers need credentialing?
Yes, most licensed providers must complete credentialing to work with insurers or hospitals.