The clean claim submission process in medical billing is the single most decisive factor affecting reimbursement speed, cash flow stability, and denial rates. According to CMS and industry benchmarks, over 20–30% of medical claims are initially denied, and nearly 65% of denials are preventable—most tied directly to errors made during claim submission.
This guide goes beyond surface-level explanations. You’ll learn how clean claims actually work in payer systems, what payers audit first, denial statistics, hidden compliance risks, and how high-performing billing teams consistently achieve 95%+ first-pass acceptance rates.
Table of Contents
ToggleWhat Is a Clean Claim in Medical Billing?
A clean claim is a medical claim that is:
-
Submitted without errors
-
Complete and accurate
-
Compliant with payer, CMS, and HIPAA rules
-
Able to be processed and paid without additional requests or manual intervention
Per the Centers for Medicare & Medicaid Services (CMS), a clean claim must not require:
-
Additional documentation
-
Corrections
-
Clarifications
-
Medical necessity reviews at intake
CMS processing benchmark:
-
Electronic clean claims: paid within 14 days
-
Paper clean claims: paid within 30 days
Why Clean Claim Submission Matters More Than Any Other Billing Step
Claim submission is not “just another step.” It is the financial choke point of the revenue cycle.
Real-World Impact
-
A 1% increase in clean claim rate can improve annual collections by $150,000–$500,000 for a mid-size practice
-
Denied claims cost $25–$118 per claim to rework (MGMA data)
-
Up to 40% of denied claims are never resubmitted, resulting in permanent revenue loss
Insight: The fastest way to improve revenue is not seeing more patients—it’s submitting cleaner claims.
What Information Is Included in a Medical Claim?
Every claim form is a legal, clinical, and financial document. Each field feeds payer adjudication algorithms.
1. Patient Information
-
Full legal name (exact payer match)
-
DOB, gender
-
Policyholder relationship
-
Reason for visit
Mismatch in patient name formatting alone accounts for ~8% of rejections.
2. Provider & Facility Information
-
Rendering, billing, and referring provider NPIs
-
Tax ID (EIN)
-
Place of service (POS)
-
Facility address
Common error: Incorrect NPI-role pairing (rendering vs billing).
3. Diagnosis & Procedure Coding
-
ICD-10-CM: medical necessity justification
-
CPT/HCPCS: services rendered
-
Modifiers (25, 59, 26, TC, etc.)
Coding drives medical necessity edits, the #1 cause of denials.
4. Charges & Units
-
Billed charge per CPT
-
Units of service
-
Line-item accuracy
Overbilling triggers audits; underbilling causes silent revenue loss.
5. Insurance Details
-
Payer ID
-
Policy number
-
Group number
-
Prior authorization references
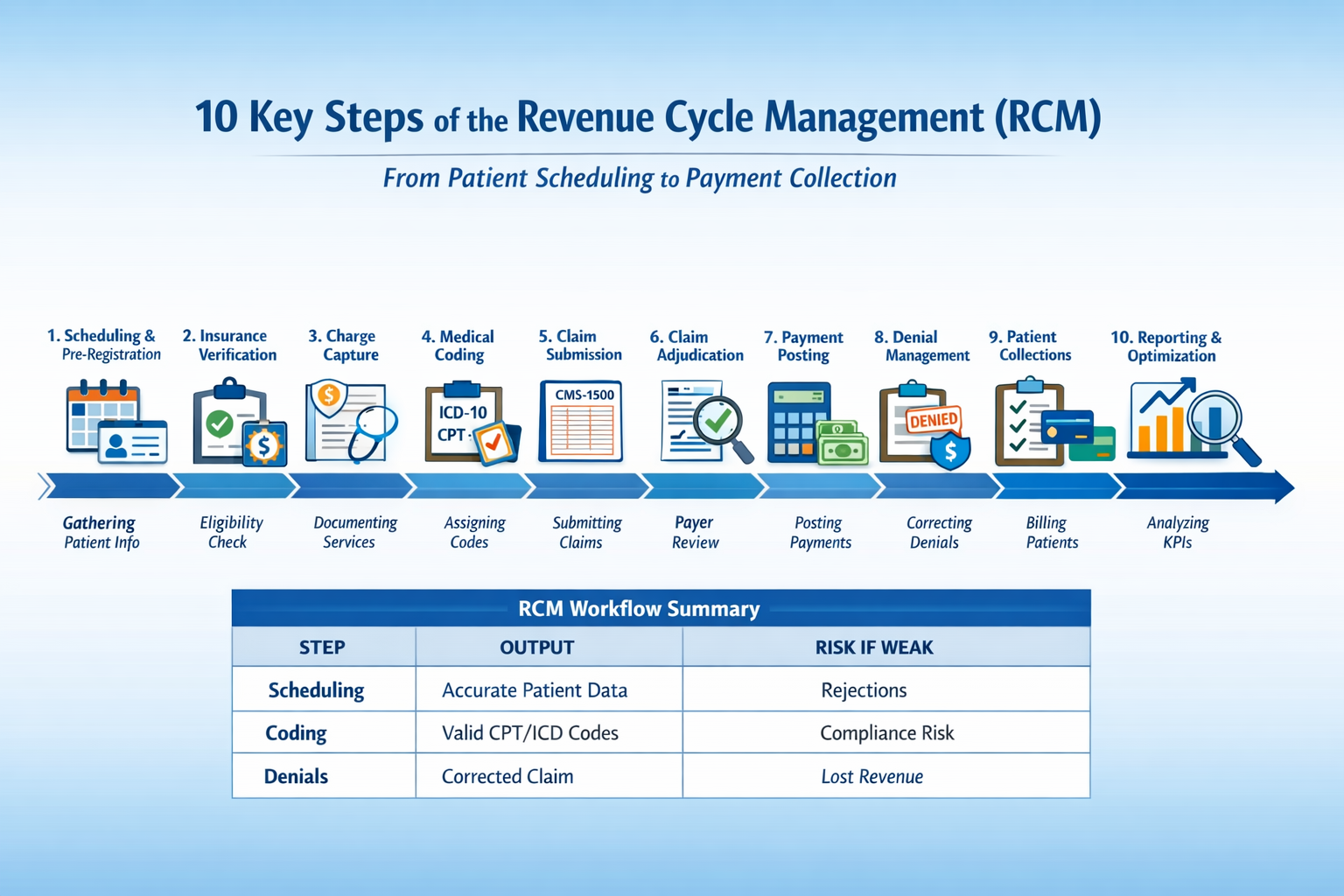
Step-by-Step Clean Claim Submission Process
Step 1: Patient Registration & Front-End Accuracy
Errors here echo throughout the revenue cycle.
Best practices
-
Real-time eligibility checks (RTE)
-
Photo capture of insurance cards
-
Verification of effective dates and coverage limits
Front-end errors cause nearly 50% of downstream denials.
Step 2: Financial Responsibility Determination
-
Copays
-
Deductibles
-
Coinsurance
-
Non-covered services
Transparent communication improves patient collections by up to 30%.
Step 3: Medical Coding (Compliance-Critical)
Professional coders translate clinical documentation into standardized codes.
-
ICD-10 supports medical necessity
-
CPT/HCPCS supports reimbursement logic
Coding accuracy directly affects payer risk scoring and audit probability.
Step 4: Superbill Creation (Out-of-Network Only)
A superbill consolidates:
-
Patient demographics
-
Provider credentials
-
ICD-10 & CPT codes
-
Dates of service and charges
Used primarily for patient-submitted reimbursement.
Step 5: Claim Scrubbing & Submission
Before submission, claims are run through scrubbing software that checks:
-
NCCI edits
-
Modifier logic
-
Payer-specific rules
-
HIPAA compliance
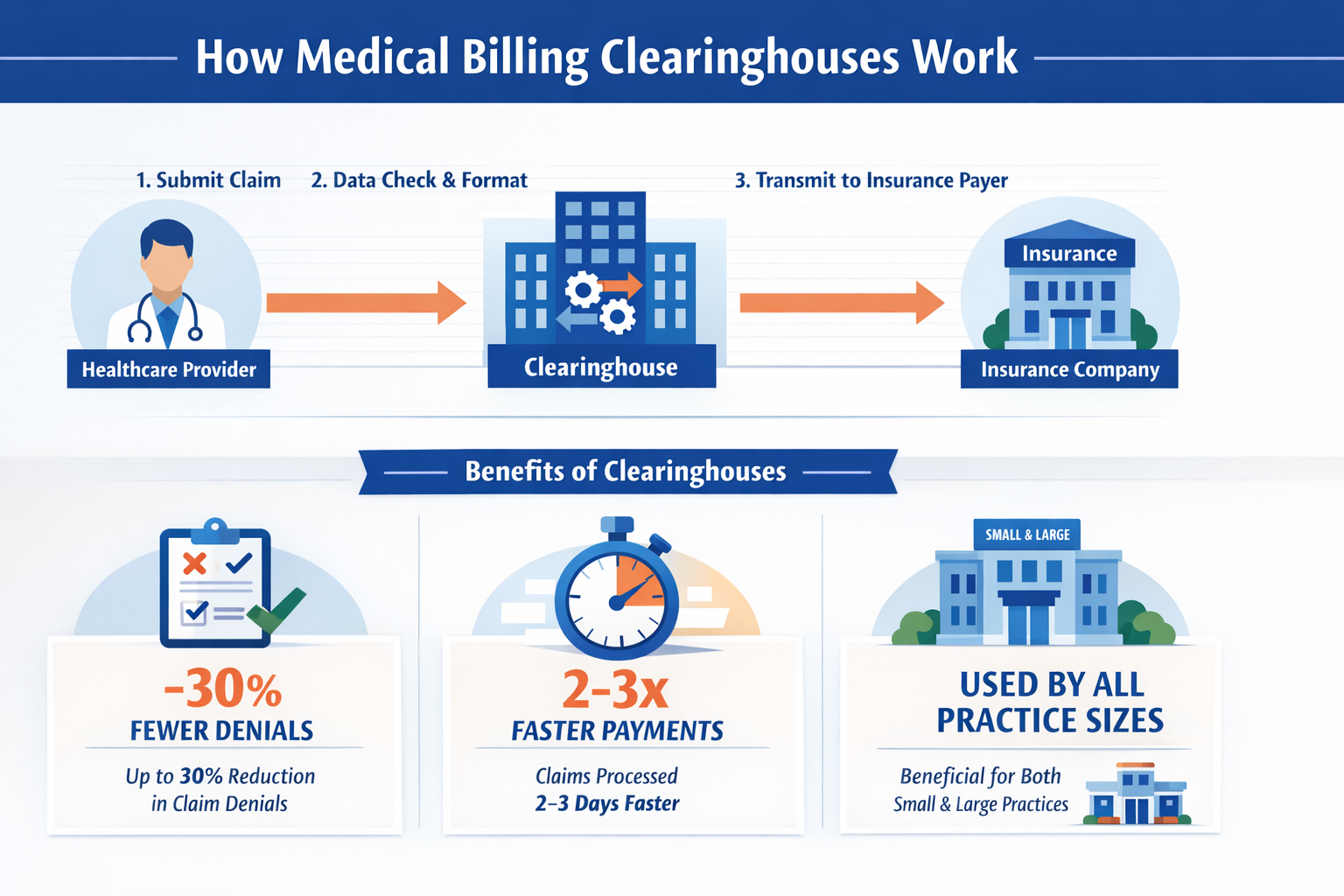
Only then is the claim submitted via:
-
Clearinghouse (electronic)
-
Mail (paper)
First-pass acceptance rate target: 95–98%
Electronic vs Paper Claim Submission (Reality-Based Comparison)
| Factor | Electronic Claims | Paper Claims |
|---|---|---|
| Processing Time | 7–14 days | 30–45 days |
| Error Rate | <5% | 15–20% |
| Tracking | Real-time | Manual |
| Cost per Claim | $1–$3 | $6–$10 |
| Audit Risk | Lower | Higher |
Over 98% of U.S. healthcare claims are now submitted electronically.
Top 12 Reasons Claims Are Denied
-
Incorrect patient or policy data
-
Coding errors or missing modifiers
-
Medical necessity not supported
-
Timely filing exceeded
-
No prior authorization
-
Services not covered
-
Duplicate claims
-
Expired policy
-
Provider credentialing issues
-
Bundling/unbundling errors
-
Place of service mismatch
-
Claim lost or not received
Key Insight: Most denials are process failures, not payer bias.
Clean Claim KPIs Every Billing Team Should Track
-
First-pass acceptance rate
-
Denial rate by payer
-
Days in A/R
-
Cost per claim
-
Rework percentage
High-performing practices review these weekly, not monthly.
Final Takeaway: Why Clean Claims Win
Clean claim submission is not about perfection—it’s about systematic precision.
-
Clean claims = faster payments
-
Faster payments = stronger cash flow
-
Stronger cash flow = sustainable practice growth
Every improvement you make in claim quality compounds financially.
In medical billing, speed follows accuracy—and accuracy starts at claim submission.