What Is EDI 837 in Medical Billing? A Simple Guide to Electronic Claims and Reimbursements
EDI 837 is the HIPAA-standard electronic format healthcare providers use to submit medical claims to payers such as insurance companies, Medicare, and Medicaid. It includes patient information, provider details, diagnosis codes, procedure codes, dates of service, and charges. The payer then processes the claim and usually responds with an EDI 835, which explains payments, adjustments, and denials.
Table of Contents
ToggleWhy Does EDI 837 Matter in Medical Billing?
If you work in medical billing, EDI 837 is one of the most important transaction formats to understand. It is the electronic version of a healthcare claim, and it allows providers to send billing data in a standardized way instead of relying on paper forms. CMS identifies the 837 as the adopted HIPAA transaction standard for electronic healthcare claims, using ASC X12 Version 5010.
That standardization is a big deal. It means a physician’s office, hospital, dental practice, or clinic can send claim data in a format that payers and clearinghouses are built to recognize and process. The result is a billing workflow that is faster, more consistent, and easier to automate than manual paper-based claims.
What Is EDI 837?
EDI 837 is the digital claim file used to bill for healthcare services. After a patient receives care, the provider’s billing system creates an 837 file and sends it electronically to a payer, often through a clearinghouse. That file tells the payer who the patient is, who provided the care, what services were performed, why they were medically necessary, and how much was charged.
Think of it this way: the 837 sends the bill, and the 835 sends the payment details back. That one distinction helps many beginners understand the medical billing workflow much faster.
What Information Is Included in an EDI 837 Claim?
An EDI 837 claim contains the core billing and clinical data needed for adjudication. Depending on the claim type, it can include patient demographics, subscriber and insurance details, provider identifiers such as NPI, diagnosis codes, procedure or service codes, dates of service, modifiers, service-line charges, and total billed amounts. CMS’s professional claim guidance and the HIPAA adopted standards pages both describe the 837 as the standard transaction used to transmit these healthcare claims electronically.
Here is the information most commonly included in an 837 file:
Who Is the Patient and What Is Their Insurance Information?
The claim includes the patient’s name, date of birth, gender, policy or member information, and the relationship between the patient and the subscriber. This data helps the payer identify coverage and route the claim correctly.
Who Rendered and Billed the Service?
The file also includes provider data such as the billing provider, rendering provider when applicable, NPI, taxonomy details in some cases, and practice or facility address information. These elements tell the payer exactly who is seeking reimbursement.
What Services Were Performed?
Service lines describe what was done and when. That usually includes CPT or HCPCS procedure codes, modifiers, dates of service, diagnosis pointers, units, and billed charges. This is the heart of claim adjudication because it connects the medical service to payment logic.
What Are the Different Types of EDI 837 Claims?
There are three main versions of the 837 transaction, and each one supports a different care setting. CMS and X12 both recognize these variations as part of the healthcare claim family.
What Is 837P?
837P stands for professional claims. It is used for services billed by physicians, therapists, outpatient practitioners, and other professional providers. This is the format most people associate with office visits and outpatient care. CMS’s 837P guidance specifically describes it as the standard format used by healthcare professionals and suppliers to transmit claims electronically.
What Is 837I?
837I stands for institutional claims. It is commonly used by hospitals, skilled nursing facilities, rehabilitation centers, and other organizations that bill for facility-based care. These claims often involve room charges, facility fees, and other institution-level billing elements.
What Is 837D?
837D stands for dental claims. It is used by dentists and dental organizations to submit oral health claims electronically. X12 documentation identifies dental claims as one of the core 837 implementations used to submit claims to primary, secondary, and subsequent payers.
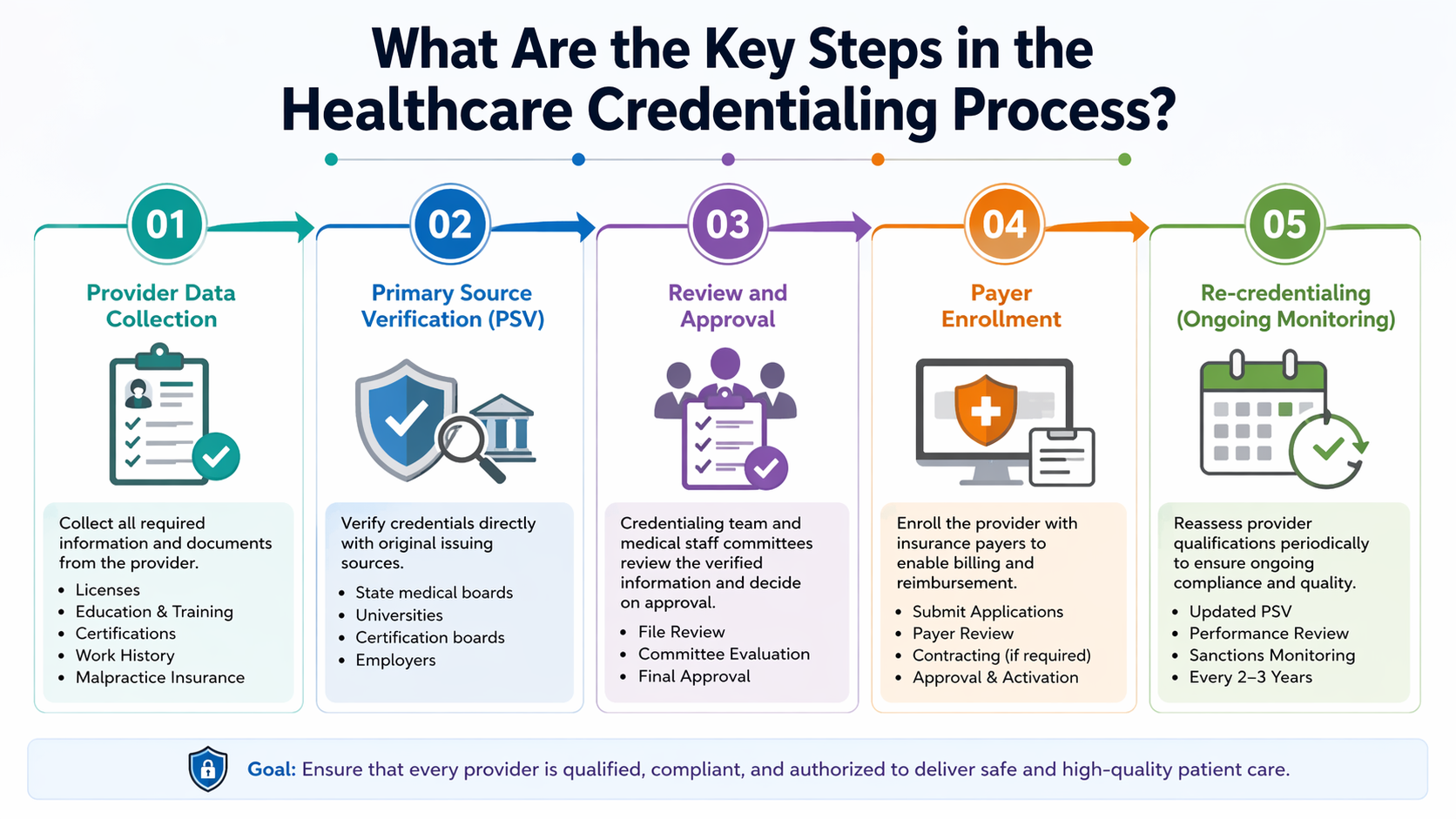
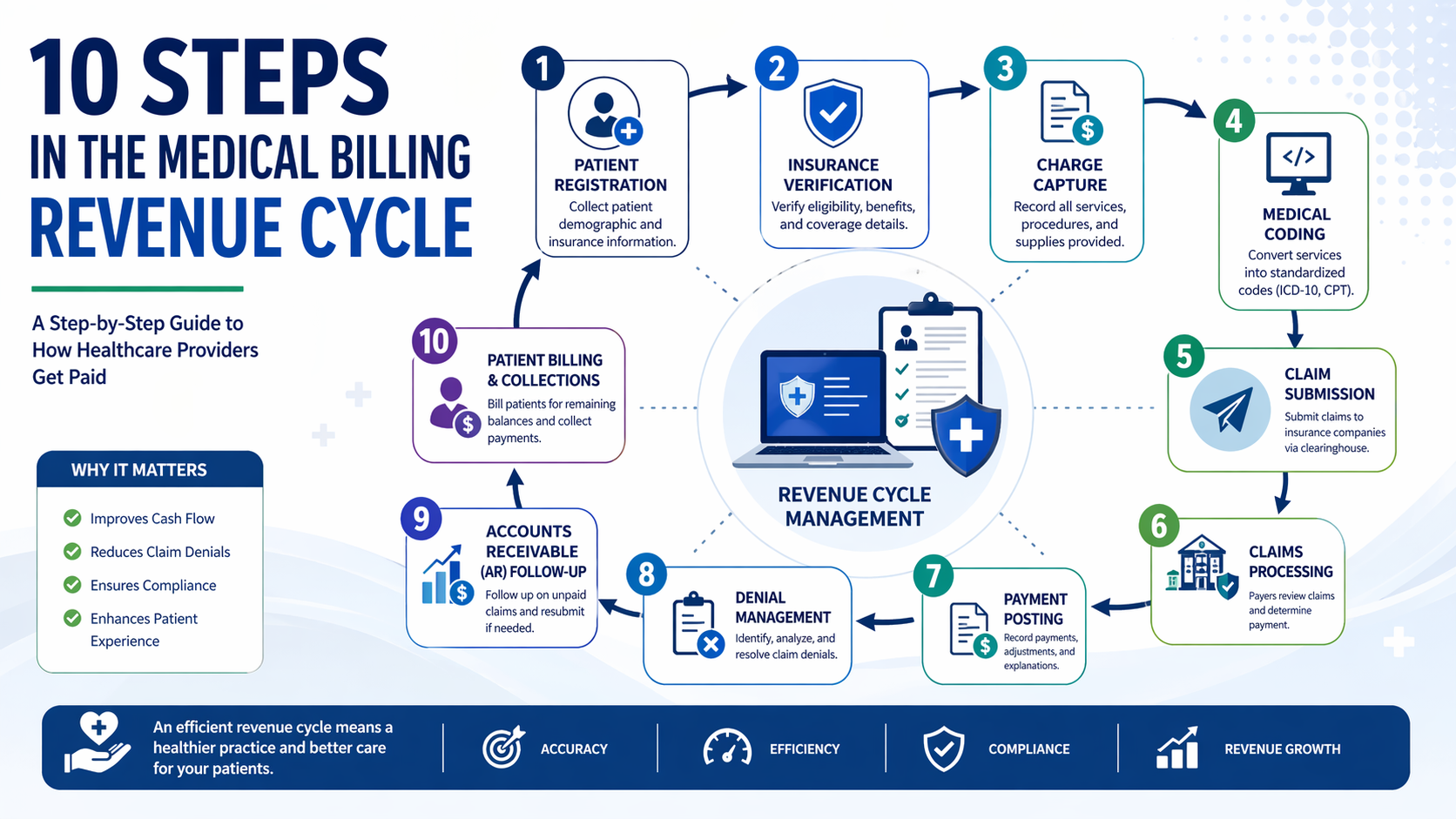
How Does the EDI 837 Workflow Work?
The basic workflow is easier to follow when you break it into steps.
What Happens First?
After the patient encounter, the provider’s billing team reviews documentation and coding. The practice management or billing system then prepares the claim using the required claim data.
What Happens Next?
The claim is converted into the EDI 837 format and sent electronically, usually through a clearinghouse. The clearinghouse checks the file for formatting issues, missing data, and common submission errors before forwarding it to the payer. This step helps reduce rejections before the claim reaches the insurance company.
What Happens After the Payer Receives the Claim?
The payer adjudicates the claim. In other words, it reviews the submitted data, applies policy and contract rules, determines allowed amounts, and decides whether to pay, reduce, or deny the claim. After that, the payer typically returns an EDI 835 remittance advice and, when applicable, a payment via EFT.
What Is the Difference Between EDI 837 and EDI 835?
This is one of the most searched questions in medical billing, and the answer is straightforward.
EDI 837 is the electronic healthcare claim submission.
EDI 835 is the electronic remittance advice that explains how the claim was processed and paid.
So when a provider asks for reimbursement, the 837 is sent out first. Once the payer reviews the claim, it sends back the 835 to show payment amounts, adjustments, denials, contractual write-downs, and patient responsibility, such as copays, coinsurance, or deductibles. CMS identifies the 835 as the adopted HIPAA standard for claim payment and remittance advice.
What Does an EDI 835 Include?
An EDI 835 contains the financial response to the claim. It typically includes claim status, the billed amount, the allowed amount, the paid amount, adjustments, denial or remark codes, and the part the patient owes. CMS’s Medicare remittance guidance notes that the 835 Version 5010A1 is the required standard for electronic remittance advice.
That is why the 835 matters so much for revenue cycle teams. It gives billing staff the information they need to post payments, reconcile accounts, identify underpayments, and work denials more efficiently.
What Do the Latest Statistics Say About Electronic Claims and Remittance?
The latest CAQH Index data shows just how dominant electronic claim submission has become. In the 2023 CAQH Index report, fully electronic claim submission reached 98% in the medical industry and 87% in the dental industry.
CAQH also estimated that moving the remaining volume to fully electronic claim submission could unlock about $2.4 billion in annual savings opportunities across medical and dental workflows.
The same report found that fully electronic remittance advice adoption reached 88% in medical and 36% in dental. CAQH estimated about $1.02 billion in additional annual savings opportunities if remaining remittance activity shifts to more fully electronic workflows. That gap suggests many organizations have digitized claim submission faster than payment posting and remittance reconciliation.
What Can We Learn from the Data?
The data tells a clear story: electronic claims are already the norm, but many revenue cycle teams still have room to improve on the payment side. Claim submission is highly digitized, yet remittance automation is not equally mature across all sectors, especially dental.
That means practices that optimize both 837 claim submission and 835 remittance posting can still gain meaningful efficiency, lower administrative costs, and shorten payment cycles. This is an inference based on the CAQH adoption and savings data.
There is also supporting operational evidence from CAQH CORE materials showing that EDI-driven claims workflows can reduce manual transactions and administrative overhead.
One CAQH CORE implementation brief reported 55% cost savings from shifting claim-status workflows from manual or web methods to EDI in a national health plan use case. While that study focused on claims processing support functions rather than 837 submission alone, it reinforces the broader value of standardized electronic transactions.
Why Is EDI 837 Important for HIPAA Compliance?
EDI 837 is not just a best practice. It is part of the HIPAA administrative simplification framework for covered entities that conduct these transactions electronically. CMS states that ASC X12 Version 5010 is the adopted standard format for these healthcare transactions, including claims and remittance advice. That is why medical billing teams must follow structured transaction standards rather than sending unformatted or proprietary claim data.
In practical terms, that means EDI 837 helps providers meet regulatory requirements while also making billing more scalable and less error-prone. Compliance and efficiency are working together here, not against each other.
Why Do Providers Prefer EDI 837 Over Paper Claims?
Providers prefer EDI 837 because it is faster, more standardized, and easier to automate than paper claim submission. Electronic claims reduce rekeying, support clearinghouse edits, improve consistency, and integrate more smoothly with billing systems and payer platforms. CMS’s transition materials for Version 5010 explain that the newer standards tightened business rules and improved data handling, thereby helping claims and remittance workflows operate more reliably.
For billing teams, the advantages typically manifest in three ways: fewer avoidable errors, faster processing, and greater visibility into the claim lifecycle. That is exactly why EDI remains foundational in modern revenue cycle operations.
FAQs
What is EDI 837 in medical billing?
EDI 837 is the HIPAA-standard electronic format used to submit healthcare claims from providers to payers for reimbursement. It includes patient details, provider data, diagnosis codes, procedure codes, dates of service, and charges.
What is the difference between 837 and 835?
The 837 is the outbound claim file. The 835 is the payer’s remittance advice that explains what was paid, adjusted, denied, or assigned to the patient.
What are the three types of 837 claims?
The three types are 837P for professional claims, 837I for institutional claims, and 837D for dental claims.
Is EDI 837 required by HIPAA?
For HIPAA-covered entities conducting standard electronic healthcare claim transactions, CMS identifies the 837 under the adopted ASC X12 Version 5010 standards.
Who uses EDI 837?
Doctors, hospitals, clinics, therapists, facilities, dentists, clearinghouses, and health plans all interact with EDI 837 transactions as part of the healthcare billing ecosystem.
Final Takeaway: What Should You Remember About EDI 837?
If you remember just one thing, remember this: EDI 837 is the standard electronic claim format that starts the reimbursement process in medical billing. It sends the payer everything needed to review the claim, and the payer responds with an EDI 835 to explain the payment outcome. Together, these two transactions form the core of the electronic medical billing workflow.